Tongue and lip tie (often abbreviated to TT/LT) have become buzzwords among lactation consultants bloggers and new mothers. For many these are strange new words despite the fact that it is a relatively common condition. Treating tongue tie fell out of medical favour in the early 1950s. In breastfeeding circles, it was talked about occasionally, but until recently few health care professionals screened babies for tongue tie and it was frequently overlooked as a cause of common breastfeeding difficulties.
In the last few years tongue tie and the related condition lip tie have exploded into the consciousness of mothers and breastfeeding helpers. So why all the fuss about tongue and lip ties all of a sudden? Tongue tie seems to be a relatively common problem, affecting 4-11%1 of the population and it can have a drastic impact on breastfeeding. The presence of tongue tie triples the risk of weaning in the first week of life.2
Here in Alberta it has been challenging to find competent assessment and treatment, prompting several Alberta mothers and their babies to fly to New York in 2011 and 2012 to receive treatment. The dedication and persistence of these mothers has spurred action on providing education and treatment options for Alberta families.
In August of 2012, The Breastfeeding Action Committee of Edmonton (BACE) brought Dr. Lawrence Kotlow to Edmonton to provide information and training to area health care providers. The attendees included; nurses, midwives, doctors, lactation consultants, dentists, and doulas. This event was just the beginning of bringing more comprehensive treatment options to our province.
What is Tongue Tie?
Tongue tie, also known as ankyloglossia, is a remnant of embryological tissue (frenum) that interferes with normal oral functions and causes a wide range of symptoms affecting untreated babies, children and adults. Lip tie is an abnormal attachment of the lip (labial frenum) to the gums (maxillary gingival tissue), which causes restricted mobility, affecting the baby’s ability to create a seal around the breast. This attachment can result in maternal and infant pain, and symptoms associated with poor milk transfer. Treatment of tongue tie (frenotomy*, clip, release, revision) involves a division or release of the membrane from the floor of the mouth.
Although the history and treatment of tongue tie is well documented, lip tie is a newer area of study with emerging data.
History of Tongue Tie
Tongue tie is documented as far back as biblical times, but in the last 70 years diagnosis and treatment have fallen out of favour. As recently as 2011, the Canadian Paediatric Society (CPS) issued a position statement about tongue ties, discouraging treatment:
Ankyloglossia (or tongue-tie) is a relatively uncommon congenital anomaly defined by an abnormally short lingual frenulum. Associations between tongue-tie and breastfeeding problems in infants have been inconsistent, and are a longstanding source of controversy in the medical community. Definitions of ankyloglossia vary, and management suggestions are not based on randomized controlled trials. Surgical correction involves cutting the lingual frenulum (frenotomy). Based on current available evidence, frenotomy cannot be recommended. If, however, the association between significant tongue-tie and major breastfeeding problems is clearly identified and surgical intervention is deemed necessary, frenotomy should be performed by a clinician experienced with the procedure and with appropriate analgesia. More definitive recommendations regarding the management of tongue-tie in infants await appropriately designed trials.3
Historically, midwives would keep a sharpened fingernail and use it to sever any tongue tie an infant might have. More recently, when childbirth in North America was the purview of general practitioners (up to the 1950’s), frenums would be routinely cut during a baby boy’s circumcision, and all baby girls would have been checked for tongue tie, having their frenums released as well. Birth becoming the purview of obstetricians as surgeons, coincided with the appearance of formula sales representatives on labour and delivery units, and the skill of diagnosing ankyloglossia and performing simple frenotomy was not passed along to obstetricians.
Today, a few dedicated health care providers still perform frenotomy, but many more have never heard of it and others believe it is of no benefit to infants. It can be heartbreakingly challenging for a parent trying to find help for tongue and lip tied babies, and mothers know that this condition impacts breastfeeding despite the CPS position statement.
There are often questions as to why we are hearing about tongue tie so much these days. Breastfeeding initiation rates have increased, so more mothers are continuing to breastfeed through challenges. Mothers are seeking solutions to breastfeeding problems and are demanding that healthcare professionals don’t give up on them. Through social media, awareness about issues like tongue tie seems to be spreading even more quickly than before. When more women are breastfeeding and talking about it online, it increases the awareness of relatively common issues that can impact the breastfeeding relationship, even if there isn’t an increase in incidence.
There are some theories, and beginning research about environmental causes relating to tongue and lip tie, and other theories about gene mutation being involved. These are questions still awaiting answers.
There is renewed interest in research about tongue and lip ties and this is forming a body of knowledge that can support health professionals and parents.
The Research
Studies and scholarly articles dating as far back as 19484 document ankyloglossia’s impact on infant feeding. More recently, these studies show a host of symptoms experienced by mother and baby and go on to identify frenotomy as an effective procedure for correcting the structural element of ankyloglossia, improving maternal comfort and increasing breastfeeding competency.5
In a 2011 review of the literature the authors found that:
Generally, performing frenotomy for ankyloglossia was associated with improvements in breastfeeding characteristics. 67.2% (275/409) of infants were breastfeeding at three months post-frenulotomy. Maternal nipple pain was significantly reduced following frenulotomy in all studies at follow-up. A significant improvement in an objective measure of latch (LATCH** score6) was demonstrated in two of the three studies using this outcome measure.7
The authors of this review felt that a randomized controlled trial of the effectiveness of frenotomy through six weeks post procedure is needed
A 2006 study randomized 25 infants to either: a) a frenotomy, assessment, sham (placebo) procedure, and assessment or; b) a sham procedure, assessment, frenotomy, and assessment. The study’s results concluded that there was a significant decrease in pain and an improvement in LATCH scores in all infants after frenotomy, but not after the sham procedure. They encountered no significant side effects and very little bleeding during frenotomy.8
Another randomized study, published in 2011, followed 58 infants who were initially randomized to two groups, frenotomy or sham procedure. The frenotomy group reported a significant decrease in nipple pain and improved infant breastfeeding scores, immediately after the procedure and again at two weeks post frenotomy. The sham group was offered frenotomy at their two week follow up appointment and all but one accepted the procedure. The babies were followed for a full year post frenotomy and continued to benefit from the reduction in pain and improvement in breastfeeding as reported in the study.9
A 1995 case report by Dianne Wiessinger is one of the earliest discussions of lip tie in the literature.10 It is also described, in 2004, in an article by Dr. Elizabeth Coryllos, as being one of many oral frenums that may interfere with lip flanging and may need treatment depending on the baby’s ability at the breast in relation to lip positioning.11 She noted that it appears in conjunction with tongue tie and may be part of a wider range of midline defects.
Dr. Lawrence Kotlow recently published a paper in the Journal of Human Lactation on “Diagnosing and Understanding the Maxillary Lip Tie as it Relates to Breastfeeding.”12 It is the first full paper to provide insight into the effect of lip ties on breastfeeding and their management. The paper also includes diagnostic criteria, a classification scale and a full explanation of the mechanics involved in upper lip flanging, gape and the impact on breastfeeding. Dr. Kotlow has performed revisions on over 1000 infants, starting treatment 40 years ago!
Long Term Implications for Not Treating
There are many potential consequences of not treating tongue and lip ties. It can be hard to foresee which problems the future may present to a tongue and lip tied individual. Because addressing the problems caused by tongue and lip ties crosses many disciplines, consensus about when to treat is lacking, and at times hotly debated. Some advocate for immediate infant revision, others encourage a wait and see treatment approach depending on how the ties impact breastfeeding, and further development. The relative skill and experience of the person performing the revision may be part of the decision to get immediate or delayed treatment. We know that all people with tongue ties are compensating for the lack of mobility (restricted function), to one degree or another, and over time the ability to effectively compensate can be compromised due to effects of aging, accident or injury.
Screening vs. Assessment
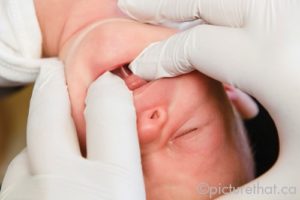
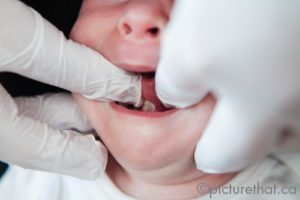
Many involved in the care and treatment of infants advocate for routine neonatal screening for tongue ties. A simple screen involves inserting a gloved finger in the infant’s mouth between the tongue and the floor
of the mouth. The finger is positioned as far back along the gums as the space where the first molar will be, and then slid from one side of the floor of the mouth to the other. If any restriction is felt (wall, membrane, or “speed bump”) the infant would be referred for a more thorough and qualified assessment of tongue structure and function as well as breastfeeding assessment and support. This is important as it is reported that 25-50% of those with structural ankyloglossia will experience breastfeeding difficulties and may require frenotomy.13
A full assessment involves a detailed examination of the infant’s oral cavity. The practitioner will be knee to knee with the parent or assistant and place the baby’s head in their lap, with the baby’s feet pointing away from them. This knee to knee position provides for optimal visualization.
The assessment will look at structure, function and symptoms. The structural assessment tells the practitioner where the membrane under the tongue is attached to the floor of the mouth. However, it does not give any information about how minor or severe a mother’s and baby’s symptoms may be. There are several classification systems for tongue tie (only one for lip tie) and some controversy as to which one is the most effective to use and where to use it. The classification information about the structure is not typically relevant to parents, but the findings of a functional assessment can be quite helpful.
A functional assessment should involve observations of the infant at the breast, calm and awake, and while sucking on the examiner’s finger (with and without milk in the baby’s mouth). It may include pre- and post-feed weights and using a stethoscope to listen to swallow sounds at the baby’s neck (cervical auscultation) to assess milk transfer and the degree of ease with which the infant swallows (bolus handling). The examiner will look for range of motion and mobility of the tongue, how widely the baby can open his mouth at the breast (gape) and how well his lips seal to the breast (flange). They will also look for signs of feeding stress in the infant. This may include: splayed fingers and toes, hands up near the face in a “warding off” position, worried or wrinkled brow, and gaze aversion. How the whole baby moves and feeds as a whole will also be observed to rule out the involvement of other issues that may be affecting breastfeeding. This would include taking a detailed history. A good assessment will always begin with a firm grounding in the normal mechanics of breastfeeding with the assessor noting any deviations from the norm. You should be able to request a copy of your assessment for your records and to take with you to the treatment provider.
Treatment Options
Treatment of tongue tie (frenotomy, clip, release, revision) involves a division or release of the membrane from the floor of the mouth and can be performed by midwives, nurse practitioners, doctors (ranging from family doctors to ear, nose and throat specialists and plastic surgeons) and dentists. As the membrane is non-vascular there is very little blood, and the procedure itself is usually quick and straightforward to perform. Revision can be performed using scissors, scalpel or laser. Alberta Health Care covers scissor revision, but not laser revision. Release of lip tie can involve more blood and swelling as this tissue is more vascular. It can be performed by the same practitioners using the same instruments as for frenotomy.
When the practitioners are highly skilled, we see no difference in the treatment methods (laser vs. scissor). Laser treatment has been reputed to have an increased incidence of post revision oral aversion, but there is currently no research to back this up. Dr. Greg Notestine recently spoke at the International Affiliation of Tongue Tie Professionals (I.A.T.P.) 2013 summit, on “Laser vs. Scissor; Deep vs. Shallow; Anesthetic or None: What Frenotomy Treatment Decisions are Best?” He said that when a practitioner was already skilled with a laser, learning to perform a frenotomy with laser was easier and there is less difficulty in achieving a complete release. “Unfortunately,” Dr. Notestine says, “the learning curve is long. But until you treat a few and get a sense of the difference from the Mom, you don’t know if your treatment/release is successful. My real test, laser or scissor, is for me to swipe the wound while treating. If it still feels like a wall of tissue, I release a little deeper until the wound feels flat. With scissors, vision is obscured by blood but can still feel. With laser I can see AND feel, but it takes 10-30 seconds to complete versus two seconds with scissors. With a screaming, squirming kid 30 sec seems like an hour!”***
When practitioners are beginning their frenotomy practice we sometimes see incomplete revision as a result of conservative treatment. For those using scissors it can be challenging to gain the confidence needed to revise far enough without fear of excessive bleeding or damaging adjacent structures. A too shallow clip or incomplete revision can sometimes increase challenges as the mechanical force of the tongue has been transferred to a smaller load. This often means that part of the tongue has more range of motion, but further back it is still restricted, leading to further difficulties with normal function.
Since the understanding of a lip tie’s potential impact on breastfeeding is so new, many practitioners are skeptical about treatment, especially with scissors or scalpel, where bleeding would be more of a concern. There is significant anecdotal evidence to encourage this treatment and a need for further research into this area.
From a practical perspective, getting to revision can be challenging. Dentists remain the easiest self-referring care provider for parents to access province wide. The downside to this is that parents expecting a quick fix can get a revision without having any breastfeeding assessment, support, or follow up care or bodywork (craniosacral therapy, chiropractic or osteopathic care, which helps the baby learn to use his newfound mobility more effectively and quickly). This experience decreases the effectiveness of the revision (sometimes causing more problems than it solves) and gives the treatment a bad reputation, supporting the view of those who think this is unnecessary, or over prescribed surgery.
Without easy access to a supportive care provider, parents are often caught trying to navigate the public health system, fighting against the stigma of the CPS position statement. There are some self-referring breastfeeding clinics in Calgary and Edmonton that provide frenotomy and some are even revising lip ties as well. When seeking treatment options look for care providers that offer a thorough assessment and are interested in being a part of a comprehensive care team including the parents, breastfeeding support and bodywork.
This Isn’t Simple
Being a new mom, struggling with breastfeeding and trying to find care can be daunting tasks. Treatment of tongue and lip ties can be complex. As with many surgical procedures, treatment of oral ties, involves more than just surgery. Assessment and skilled (often ongoing) breastfeeding support are part of comprehensive care combined with pre and post revision bodywork, and post revision physical therapies for the babies.
All wounds are inclined to heal themselves closed and the frenotomy site is no different. In order to avoid healing reattachment, the parents need to commit to performing routine stretching exercises which can be stressful. This practice is hotly debated among professionals, but there is now some research coming to back up post frenotomy stretching.14 The person performing the frenotomy should provide a list of post-surgical care and stretching instructions, and the parents should be committed to performing the stretches before the revision is considered. We see improved results and less need for repeat revisions with stretching routines.
Some babies may need specific suck retraining exercises in order to relearn correct use of the tongue and other muscles used for feeding and swallowing. A skilled breastfeeding support person can determine the exact types of exercises need to achieve normal range of motion and effective nursing skills.
Bodywork: What is it and why is it important?
Babies can present with breastfeeding challenges as a result of a difficult birth (vacuum, forceps, Caesarean section, long or difficult pushing stage) or being constricted in utero (breech, transverse lie, posterior presentation, uterine scarring, multiple pregnancy), or a congenital abnormality such as tongue tie.
Bodywork refers to different types of gentle, non-invasive, manual therapies that can be used to help treat and correct breastfeeding problems with underlying structural causes. Practitioners can include: chiropractors, osteopaths, massage therapists, physical therapists, and craniosacral therapists. These manual therapies are particularly useful in helping to treat tongue and lip ties, before revision, instead of revision, and during recovery and healing after a revision.
As the tongue forms in utero it shapes the palate, which in turn shapes the sinuses. The rest of the craniofacial structures follow suit. A tongue that is restricted in utero by a frenum, does not allow for normal oral development, and tongue tied babies are often born with abnormalities of the palate and other craniofacial structures (i.e. narrow nasal passages). Torticollis (a muscular condition where the neck muscles are restricted causing the head to tilt in one direction) is sometimes seen in conjunction with tongue tie. The tongue tie often holds tight the surrounding muscles of the face head and neck.
Having bodywork prior to revision can loosen and normalize the surrounding structures to such an extent that the tie is no longer problematic. Allison Hazelbaker describes this phenomenon as “faux tie”, when constricted muscles cause the appearance of a significant frenum that reduces with bodywork.
Manual therapy can release the muscle tension and allow for more of the tie to “come forward” in the mouth, making it easier for the revising practitioner to get a complete revision. Some bodyworkers can provide a diagnosis of ankyloglossia that may be difficult to obtain in the conventional medical system. Pre-revision care often includes multiple visits close together (i.e. four to six visits, every second day) then decreasing over time when improvement is made.
One of the markers of a tongue tie in need of revision is that the baby does not improve with skilled bodywork. Following a course of bodywork treatment to see if the results of the treatment are lasting can sometimes be a test to see if revision is needed. The tongue tie requiring treatment will continue to pull the surrounding structures out of alignment over time. Babies who respond well to body work, but regress quickly might be good candidates for revision.
Post-surgical body work is important too. Manual therapy can help the body to adjust to its new range of motion, and even deal with some of the trauma associated with the revision process. Craniosacral therapy (CST) is particularly good for this and the CST practitioner will often treat the mother and baby at the same time allowing the mother to release trauma she may be holding relating to unsuccessful or stressful breastfeeding experiences.
Some bodyworkers recommend seeing the baby as soon as possible after revision, and again after a one to two day interval, decreasing treatments over time with improvement. The bodyworker can be an important part of the care team working in conjunction with, and as a complement to, services provided by a skilled breastfeeding support worker.
Healing and Relearning
The time post revision can be a trying one for parents, juggling appointments with bodyworkers and breastfeeding support, while re-learning to breastfeed and performing stretches. Some families treat this time as they would the immediate postpartum period and have a “lying in” or babymoon during the early recovery period.
In the first day after revision, many babies are in pain and upset. Some parents use an over the counter pain reliever. Others might opt for homeopathic pain relief. Some families provide comfort measures and wait it out. Be sure to check with your care provider for appropriate pain control measures. It is not uncommon for a baby to have a temporary and usually short lived nursing strike during this time. If this happens, the mother will need to maintain her milk supply by pumping or hand expressing, and feeding the baby by an alternate method. Although some mothers notice an immediate improvement in latch and pain, many mothers do not. Getting to normal breastfeeding can be slow. Often it is only one more good feed each day post revision. Most mothers see noticeable improvement in two to four weeks. The longer the baby had the restriction, the longer it may take to recover.
During this time a mom and her family need lots of support. She may appreciate having a meal prepared, help with older children, shopping or other household tasks being taken care of so that she may focus on caring for and learning to nurse her recently revised baby. This process can be very emotionally trying for the mother, as she begins to let go of the stress of struggling to get help and copes with the mixed feelings surrounding her expectations of herself, her baby and the revision process. She may have ongoing struggles with diminished milk supply, or need to heal damaged nipples. Emotional support during this time can be invaluable, and can come from partners, family friends and professionals.
Tongue and lip ties are a relatively common problem and revision is a relatively simple procedure. But for most parents, the journey from symptoms to successful and comfortable breastfeeding is complex and overwhelming. Building a team of professional support, appropriate pre- and post-care and community support are all a part of addressing this common problem. B
* Frenotomy is sometimes described as the release of the band of tissue, whereas frenectomy is the release and removal of the membrane. However both words (as well as frenulotomy) are often used interchangeably in the literature.
** “LATCH is a breastfeeding charting system that provides a systematic method for gathering information about individual breastfeeding sessions. The system assigns a numerical score, 0, 1, or 2, to five key components of breastfeeding. Each letter of the acronym LATCH denotes an area of assessment. ‘L’ is for how well the infant latches onto the breast. ‘A’ is for the amount of audible swallowing noted. ‘T’ is for the mother’s nipple type. ‘C’ is for the mother’s level of comfort. ‘H’ is for the amount of help the mother needs to hold her infant to the breast.” (Jensen D, 1994)
*** Personal communication October 13, 2013.
Symptoms of Tongue Tie and Lip Tie in Untreated Mother/Baby Dyad
- leaking or spilling of milk from breast (or bottle)
- sucking blister(s) or callous
- noisy feeds, clicking, snapping or slurping sounds
- maternal (and infant) pain
- reflux
- colic
- low, slow weight gain, failure to thrive
- infant slides off the nipple
- chomping or chewing on the nipple
- tongue and jaw tremors (indicate fatigue)
- falls asleep at the breast before fully fed
- baby exhibits signs of stress (during feeds)
- sputters, gags, chokes
- breast refusal
- picky nurser (will only nurse in certain positions or locations)
- nipples appear flattened, blanched or creased post feed
- cracked, bruised or chafed nipples
- bleeding nipples
- pain with latch or throughout feed
- incomplete breast drainage
- plugged ducts/mastitis
- thrush or bacterial infection
- lack of hormone surge
Symptoms Associated with Tongue and Lip Tie In Children and Adults
- persistent reflux
- snoring and sleep apnea
- difficulty with speech and articulation
- dental caries (cavities)
- problems with developing orthodontia
- narrow, high palate
- migraines
- TMJ disorders
- chronic pain
- chronic sinus infections (looks like allergy)
- feeding and swallowing problems
- diastema (gap between the upper front teeth)
Resolving Tongue-Tie: One Family’s Journey
References
- Hazelbaker, A. (2010). Tongue Tie: Morphogenesis, Impact, Assessment and Treatment. Aidan and Eva Press.
- Ricke, L. A., Baker, N. J., Madlon-Kay, D. K., & DeFor, T. (2005, January). Newborn Tongue-tie: Prevalence and Effect on Breast-Feeding. Journal of the American Board of Medicine, 18(1), 1-7.
- Rowan-Legg, A. (2011, April 1). Canadian Paediatric Society.
- May, H., & Chun, L. T. (1948). Congenital Ankyloglossia Associated with Glossoptosis and Palatum Fissum. Pediatrics, 2(6), 685-687.
- Coryllos, E., Watson Genna, C., & Salloum, A. (2004, Summer). Congenital Tongue-Tie and Its Impact on Breastfeeding. Breastfeeding: Best for Baby and Mother, pp. 1-6.
- Jensen D, W. S. (1994, January). LATCH: A Breastfeeding Charting System and Documentation Tool. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 23(1), 27-32.
- Constantine, A., Williams, C., & A.G, S. (2011). A Systematic Review of Frenotomy for Ankyloglossia (Tongue Tie) in Breast Fed Infants. Archives of Disease in Childhood, 96(Supplement 1), A62-A63.
- Dollberg S, B. E. (2006, September). Immediate Nipple Pain Relief After Frenotomy in Breast-Fed Infants with Ankyloglossia: A Randomized, Prospective Study. Journal of Pediatric Surgery, 41(9), 1598-600.
- Buryk, M., Bloom, D., & Shope, T. (2011, August). Efficacy of Neonatal Release of Ankyloglossia: A Randomized Trial. Pediatrics, 128(2), 280-288.
- Wiessinger, D., & Miller, M. (1995, December). Breastfeeding Difficulties as a Result of Tight Lingual and Labial Frena: A Case Report. Journal of Human Lactation, 11(4), 313-316.
- Coryllos, op. cit.
- Kotlow, L. (2013, November). Diagnosing and Understanding the Maxillary Lip-tie (Superior Labial, the Maxillary Labial Frenum) as it Relates to Breastfeeding. Journal of Human Lactation, 29(4), 458-464.
- Segal, L., Stephenson, R., Dawes, M., & Feldman, P. (2007, June). Prevalence, Diagnosis, and Treatment of Ankyloglossia. Canadian Family Physician, 53(6), 1027-1033.
- Demyati, S., Ankyloglossia in Breastfeeding Infants: Stretching Exercises Post Frenotomy and the Efficacy of the Procedure. In Press.
Lee-Ann Grenier is the mother of three breastfed children. She has been helping mothers breastfeed since 2005. After a ten month battle to get treatment for her tongue-tied baby, she flew to New York to see Dr. Kotlow, a pediatric dentist specializing in lip and tongue ties. She has immersed herself in the world of tongue and lip ties and her personal experience combined with her lactation expertise and holistic approach give her a unique perspective on this complex problem.
Photos by: Picture That Photography
Local Resources for Tongue and Lip Tie Revision in Alberta
This listing is for information only. It is not an endorsement of any practitioner and it is not necessarily complete or current. It is important to discuss your particular situation with your caregiver. Different practitioners will have different levels of experience and expertise and should not be asked to operate outside of their comfort zone. Qualified assessment, breastfeeding support, and pre- and post-care requirements should all be considered prior to pursuing a revision. If you have additions or changes to this listing please contact us.
BACE (Breastfeeding Action Committee of Edmonton) maintains a list of practitioners who attended training with Dr. Kotlow in August 2012.
For more information: Tongue-Tie The Best Evidence
One Family’s Tongue-Tie Journey
Laser revision of tongue and lip tied infants is being performed around the province by the following practitioners:
Breton
Dr. Hambleton
780-696-3434780-696-3434
Calgary
Dr. Lam and Dr. Lan at Westmarket Dental
339-1851 Sirocco Drive SW
403-246-8555403-246-8555
Edmonton
Dr. Bolt at Summerside Dental
#8, 1109 Summerside Drive SW
780-665-4833780-665-4833
Dr. Heit at Scotia Square Dentistry
10060 Jasper Avenue
780- 429-4968780- 429-4968
Non-Laser revision (covered by AHC) is also being offered around the province:
Calgary
Dr. Jain (prefers referral, revises TT, PTT and LT, covered by AHC) Lakeview Breastfeeding Clinic at Richmond Square
#70, 3915 – 51st Street SW
403- 246-7076403- 246-7076
24 hr. leave a message
Dr. Meldrum at Foothills Breastfeeding Clinic
#101, 1318 Centre Street North
403-266-2622403-266-2622 (extension 3) for more information.
Edmonton
Breastfeeding Clinic – Grey Nuns Community Hospital
1100 Youville Drive NW
780-735-7346780-735-7346
Referral by letter or telephone call from a physician or Registered Midwife is required.
Sherwood Park
Erica Kalke at Synergy Women’s Wellness Centre
225 Synergy Wellness Centre
501 Bethel Drive Sherwood Park AB T8H 0N2
780- 467-4343780- 467-4343
There are other practitioners in Alberta who provide frenotomy, either exclusively to their own patients, or who require a referral and sometimes significant wait times, such as ENTs and plastic surgeons.
Online support: many great supports, including references to local resources, can be found online.